Do You Have Good Posture?
Everybody wants to know: Do I have good posture?
Good posture is a valuable indicator of good musculoskeletal (muscle and joint) health. One great test of
upright posture is the “Wall angel test”. This test is a quick and easy way to assess how far your posture has been eroded by poor habits, a
sedentary lifestyle, past injuries or poor training from the upright posture we evolved to possess, to the “computer posture” so many of us
now exhibit.

To perform the Wall Angel Test:
-
Find a clear wall and stand with your back to it. Your head, mid-back and buttocks should all be touching, your feet can be a comfortable
distance (a few inches) away.
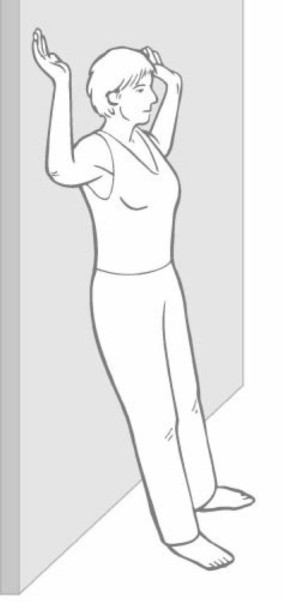
- Next bring you’re your arms up to the 90/90 position (as shown) with the back of your wrists and fingers against the wall.
- Then, without moving your head or hands, try to also flatten your lower back to the wall.
Scoring
This test can be scored from 0-3, with the results as follows:
3 – Perfect!
- You can comfortably achieve the position as shown.
- Your eyes are horizontal, not looking up, and your chin is not jutting out.
- You can simultaneously flatten your fingers, hands and spine against the wall.
-
If you are in this category well done! A ‘3’ doesn’t nessarily mean that you dont have any postural flaws but does
show you have good global movement in most of the right areas (shoulders, chest, spine). You will likely gain more benefit from
focusing on strength and stabilisation training rather than stretching exercises.
2 – Pretty good:
- You can flatten your head against the wall with your eyes horizontal and your chin not poking out.
- You can flatten your fingers and can almost flatten your wrists but not quite (<1cm form the wall).
- You can almost flatten your spine to the wall but not quite.
-
A ‘2’ translates to ‘good enough’ – not perfect, but not worth worrying too much about. Your time would be
better spent working on other areas.
1 – Work needed:
-
You can’t flatten your head against the wall or you can flatten you head but to do so your chin juts out or your eyes are no longer
horizontal.
- You can’t flatten your fingers against the wall or your wrists are still a way off (> 1cm from the wall).
- You can’t flatten your spine anywhere near the wall.
-
A ‘1’ indicates a dysfunction of upright posture. If you have neck or shoulder pain this is likely a contributing factor. If you don’t
currently have pain you are likely at higher risk for neck, shoulder or low back injury. Look out for next week’s post on exercises
you can follow to make improvements.
0 – Pain
- You experience pain during any phase of the test.
-
This test should not cause pain, if it does it is not normal. You should have it investigated by a suitable healthcare
practitioner.
A bad score does not make you a bad person! Take it for what it is – information. Use this information to your advantage and make
improvements where needed. Improvemnts in upright posture can lead to less pain, better movement and lower
risk of injury.
With a little dedication everybody can make improvements to their posture. Look out for next week’s post on some simple exercises to improve
your posture.
Are you worried about your posture? Click here to find out how we can
help.
Related articles
Images
Figures reproduced from Liebenson. C., Journal of Bodyworks and Movement Therapies
This post was written by Steffen Toates. Steffen is a chiropractor at Dynamic Health Chiropractic in Jersey CI. For more information about
Steffen click here.


Leave a Comment
It sounds like you may have excessive tightness through your chest or shoulders making it difficult to reach the starting position and meaning your shoulders are having to work extra hard to try and get there leading to the burning.